Mr Sangoma's story
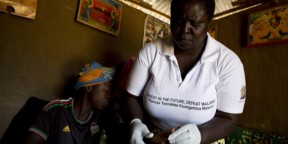
Mr. Ndibi Sangoma did not attend medical school, but those who live in his village call him doctor. He does not need a stethoscope or lab coat to save lives.
“In these 3 villages I’m called a doctor because I’ve taught them how to prevent themselves from malaria. If there is a problem [with malaria] I can be called at night to solve the problem,” he said. When a patient comes to Sangoma with problems he is not trained to address, he refers them to the Zambezi Rural Health Centre.
Sangoma has been working as a malaria volunteer, also known as a malaria control agent, in the Zambezi health facility catchment area, located in Sesheke District in Zambia’s Western Province, for nearly ten years. He was motivated to become a volunteer after suffering from malaria and subsequently receiving help from a community health worker.
“I fell sick before I joined in 2010 and a community health worker came to test me and found that I was suffering from malaria and they started administering the medication," he explains, "when I recovered, I wanted to work with him. I was chosen by the clinical office at Zambezi and then became a malaria control agent.”

In these 3 villages I’m called a doctor because I’ve taught them how to prevent themselves from malaria. If there is a problem [with malaria] I can be called at night to solve the problem.
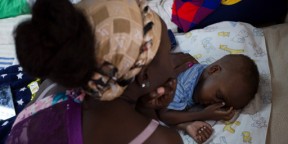
When Sangoma first became a volunteer, children were dying from malaria. Back then, parents would take their children to traditional healers because they did not understand that mosquitoes transmit malaria, he shared.
Today, malaria cases within the Zambezi health facility catchment area, comprised of multiple villages, are almost unheard of. Just three cases have been reported this year among the nearly 8,000 people who live there. The country of Zambia as a whole has witnessed similar success within the past several years; between 2016 and 2018, the country’s malaria case fatality rate dropped from 19 per 1,000 persons to 9 per 1,000 persons – and malaria incidence dropped from 381 cases per 1,000 people to 191 cases per 1,000 people.
Zambezi is on the path towards malaria elimination in part because of Sangoma and thirteen other malaria volunteers who have been trained by Zambian Ministry of Health staff, in partnership with the J.C. Flowers Foundation’s Isdell:Flowers Cross Border Malaria Initiative, to diagnose and manage malaria cases within their communities. As part of their training, the volunteers learned the dangers of the mosquito and how it can transmit malaria parasites from human to human.